When Does Superficial X-Ray Radiotherapy Make Sense in Dermatology Practice? A Practical Guide for Clinics
2026-04-15 16:59When Does Superficial X-Ray Radiotherapy Make Sense in Dermatology Practice?
Superficial X-ray radiotherapy is receiving renewed attention in dermatology, but it is often described too broadly. In real practice, the more useful question is not whether superficial radiation therapy can be used for skin lesions in general. The better question is when it makes clinical sense, for which patients, and in what kind of treatment workflow. Radiation therapy remains an accepted option in selected basal cell carcinoma and cutaneous squamous cell carcinoma settings, but it is not a universal replacement for surgery.[1][2]
That distinction matters because dermatology clinics are not simply choosing a machine. They are deciding how superficial radiation therapy would fit into diagnosis, case selection, dose planning, follow-up, and patient communication. Current guidelines and cancer care resources consistently position radiotherapy as a valid option for selected nonmelanoma skin cancers, especially when surgery is less suitable or cosmetic and functional considerations are important.[1][2][3]
Why This Topic Matters Now
Nonmelanoma skin cancer remains one of the most common malignancies in dermatology practice, and treatment decisions are not always straightforward. While surgery remains central in many cases, radiotherapy continues to have a role, particularly for selected patients who are not ideal surgical candidates or for lesions in locations where tissue preservation and cosmesis matter. ASTRO’s guideline addresses radiation therapy as both definitive and postoperative treatment for basal cell carcinoma and cutaneous squamous cell carcinoma, while Cancer Research UK and the American Cancer Society also describe radiotherapy as an option for selected skin cancers on or near the skin surface.[2][3][4]
This is also why superficial X-ray radiotherapy deserves a more practical discussion. The decision to add SRT is not just about having another treatment modality. It is about whether a clinic has the right patient mix, the right workflow, and the right expectations about what radiotherapy can and cannot do.
What Superficial X-Ray Radiotherapy Actually Does
Superficial radiotherapy uses low-energy X-rays to treat lesions on or close to the skin surface. Because the radiation does not travel far into deeper tissues, it is particularly relevant for superficial disease rather than deep or bulky tumors. Cancer Research UK explains this simply: superficial radiotherapy treats cancer on or close to the skin surface because the radiation does not travel far into the body.[3]
That depth profile is one reason SRT is discussed in dermatologic oncology. Reviews and educational sources describe it as a treatment option for nonmelanoma skin cancers such as basal cell carcinoma and squamous cell carcinoma, especially when a non-surgical approach is being considered.[2][4][5] This is also consistent with how your XT-5601 is positioned publicly: as a superficial X-ray radiation therapy system for skin lesions and selected dermatologic oncology indications, with emphasis on focused delivery and shallow penetration.
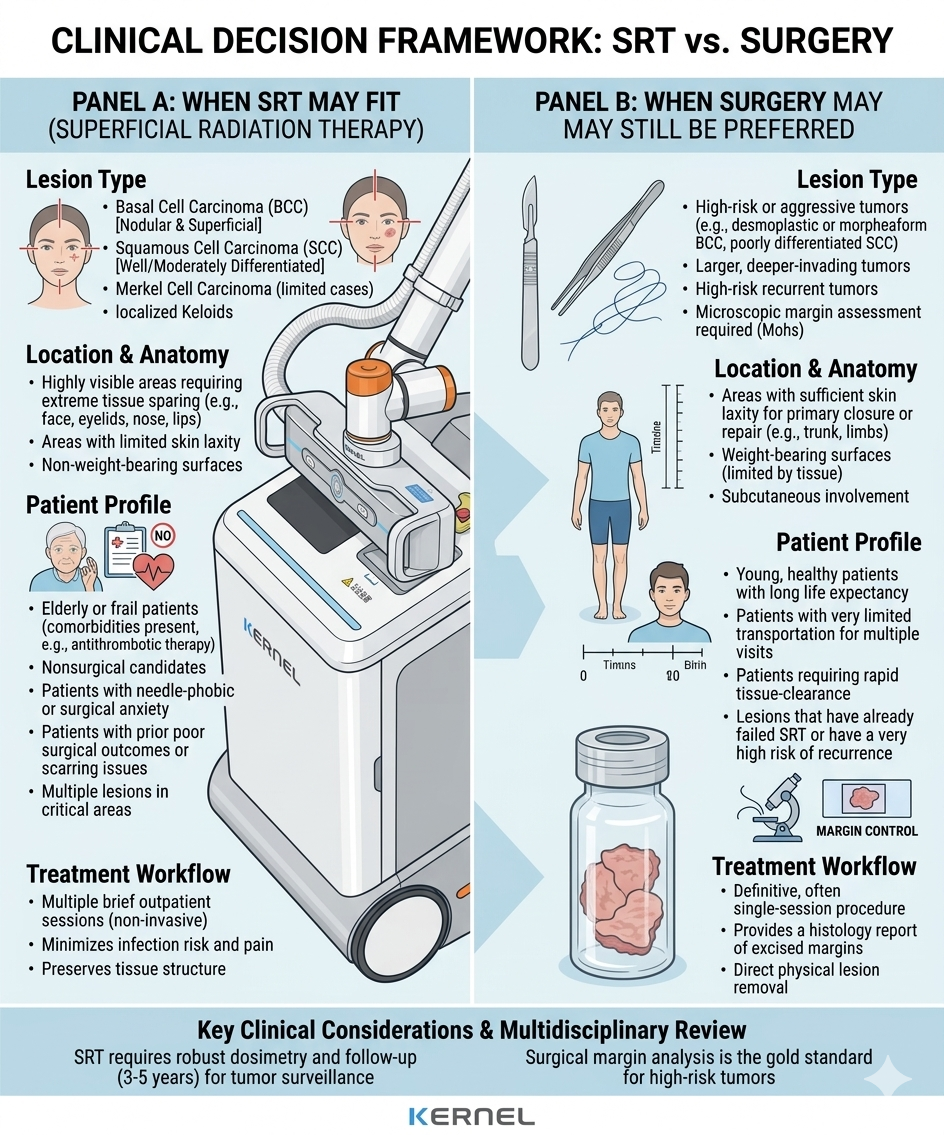
Where SRT May Be a Good Fit
Superficial X-ray radiotherapy may be a reasonable fit when surgery is not the best practical option. This can include older patients, patients with significant comorbidities, lesions in cosmetically sensitive areas, or situations where a non-surgical treatment pathway is preferred after appropriate evaluation. Public cancer resources describe radiotherapy as a treatment option for skin cancers that cover a large area, occur in difficult-to-operate locations, or affect patients who are not good surgical candidates.[4]
It may also make sense in clinics that want to build a more structured nonsurgical dermatologic oncology workflow. That does not mean replacing surgery as a rule. It means recognizing that some skin oncology cases are better served by a broader treatment menu. CMS coverage summaries referencing AAD, ASTRO, and NCCN materials note that radiotherapy can be appropriate for selected basal and squamous cell skin cancers and that many case series report local control rates above 90%, while still framing treatment selection around clinical appropriateness rather than marketing claims.[1]
For clinics actively evaluating treatment equipment, current superficial X-ray radiotherapy systems are increasingly positioned around precision delivery, shallow penetration, and practical outpatient use. That is exactly how this modality should be discussed: not as a blanket alternative for all lesions, but as a focused option within selected dermatology workflows.
When SRT May Not Be the Best First Choice
This point is essential. A useful clinic article on SRT should say clearly that not every lesion is best managed this way. In many nonmelanoma skin cancer cases, surgery remains the primary or preferred approach, especially when margin-controlled excision is important or when pathology from excised tissue plays a central role in management. ASTRO’s guidance does not frame radiation therapy as a universal first-line replacement. It defines when radiotherapy is appropriate, not when it should replace all other approaches.[2]
That is also why superficial radiotherapy should not be presented as a shortcut treatment. It requires patient selection, treatment planning, dose logic, and careful follow-up. A 2024 JAAD study on superficial X-ray treatment in nonaggressive basal cell carcinoma highlights that it may be a useful, well-tolerated alternative in select nonsurgical patients, which is a much more precise and credible way to describe the modality.[6]
What Clinics Should Evaluate Before Adding SRT
The first question is clinical fit. Does the clinic regularly see selected nonmelanoma skin cancer cases in which a nonsurgical option would be useful? If not, adding SRT may be difficult to justify operationally. If yes, the next issue is workflow: who will evaluate candidacy, who will plan treatment, how will dosing be managed, and how will follow-up be documented?
The second question is device capability. An SRT system should not be judged only by whether it uses X-rays. Positioning, output stability, console logic, treatment control, and daily usability all matter. The XT-5601 superficial X-ray radiation therapy system is presented around robotic positioning, stable radiation output, and intelligent control, which makes it more appropriate to discuss in workflow terms rather than as a generic “skin device.”
The third question is how SRT fits the clinic’s broader skin oncology pathway. Clinics that already use noninvasive imaging in skin oncology may also think about how reflectance confocal microscopy and radiotherapy planning sit within the same broader diagnostic pathway. That kind of connection is useful because it turns SRT from a standalone sales concept into part of a more coherent dermatology workflow.
Choosing Based on Workflow, Not Slogans
A superficial X-ray radiotherapy system should not be adopted because it sounds advanced. It should be adopted only when the clinic has a clear use case, understands the patient population, and can integrate the modality into real treatment planning. That is a more serious and more useful standard than broad statements about innovation.
This is also where many device articles go wrong. They compare surgery and radiotherapy as if one must fully displace the other. In reality, the more practical question is narrower: in which cases does a clinic benefit from having a superficial radiotherapy option available? Once that question is asked honestly, the article becomes more clinically grounded and more relevant to buyers.
Conclusion
Superficial X-ray radiotherapy makes the most sense in dermatology practice when it is used for the right cases, in the right setting, and with the right expectations. It can be a valuable option for selected superficial nonmelanoma skin cancers and other superficial lesions when surgery is less suitable or when a nonsurgical workflow is clinically justified. But it should be adopted as part of a thoughtful treatment pathway, not as a catch-all alternative.
Explore KernelMed's superficial X-ray radiotherapy solutions for selected dermatology and skin lesion treatment workflows.
FAQ
What is superficial X-ray radiotherapy used for in dermatology?
It is used for selected lesions on or near the skin surface, including selected nonmelanoma skin cancers and other superficial dermatologic indications, depending on clinical judgment and treatment planning.[2][3][5]
Is SRT a replacement for surgery in skin cancer treatment?
No. Surgery remains primary in many cases. Radiotherapy is a valid option in selected settings, especially when surgery is less suitable or when cosmesis and function are major concerns.[2][4]
Which patients may be good candidates for superficial radiotherapy?
Selected nonsurgical candidates, older patients, some patients with lesions in cosmetically sensitive areas, and certain patients for whom an outpatient radiotherapy workflow is more appropriate may be considered.[2][4][6]
What should clinics evaluate before adding an SRT system?
Clinical case mix, treatment workflow, device capability, positioning accuracy, output stability, and follow-up pathway are all important.
Why is shallow penetration important in superficial X-ray therapy?
Because the goal is to treat lesions near the skin surface while limiting dose to deeper tissues.[3][5]
References
[1] CMS. Superficial Radiation Therapy (SRT) for the Treatment of Nonmelanoma Skin Cancer.
[2] ASTRO. Skin Cancer Guideline.
[3] Cancer Research UK. Superficial radiotherapy to the skin.
[4] American Cancer Society. Radiation Therapy for Basal and Squamous Cell Skin Cancers.
[5] Han H, et al. Superficial radiation therapy for nonmelanoma skin cancer: a review.
[6] Mattia A, et al. Superficial X-ray in the treatment of nonaggressive basal cell carcinoma. JAAD, 2024.